November is Prematurity Awareness Month. Since 2003, the leading prematurity awareness organization has raised funds and worked to protect moms and babies against preventable preterm births—but what about the unpreventable preterm births? What about me?
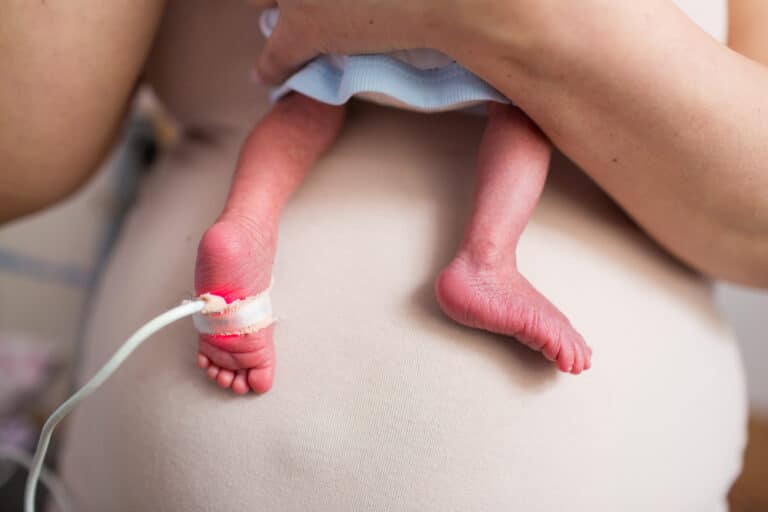
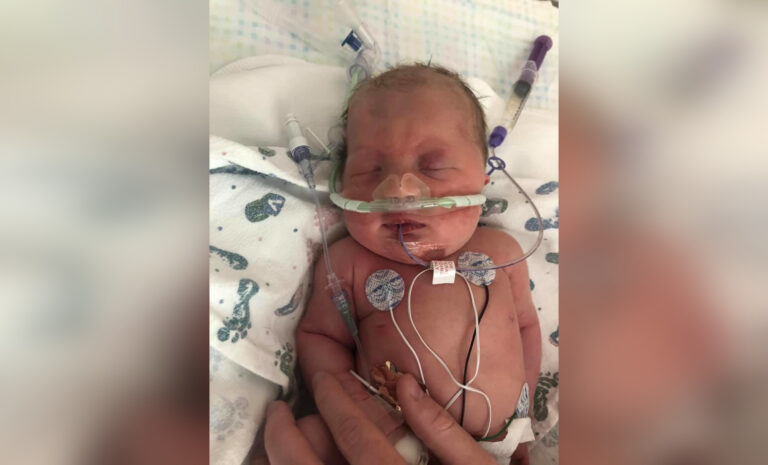
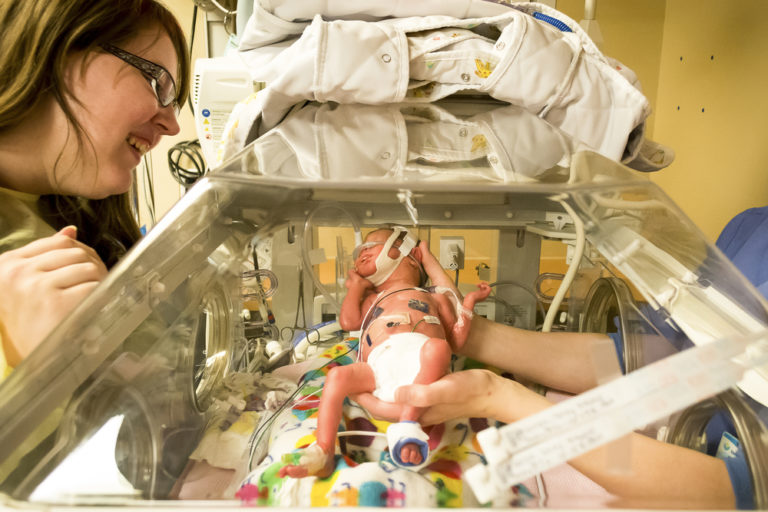
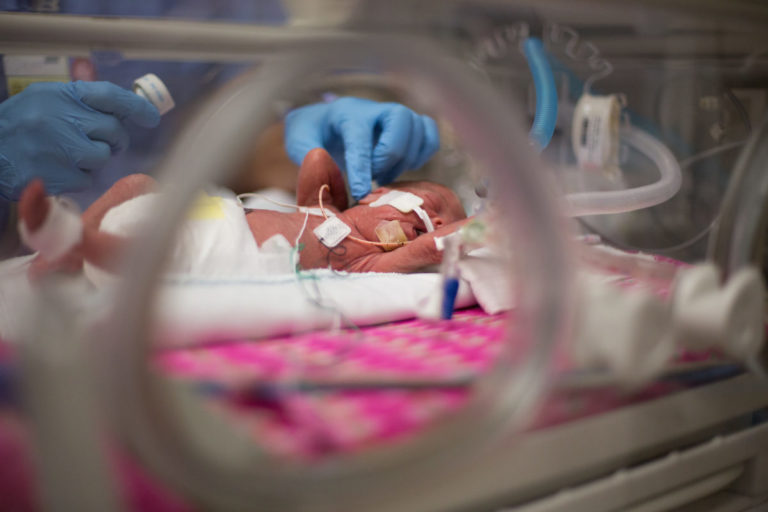
On December 15, 2019, my daughter arrived 17 weeks and two days early. Two days later, her little sister, and identical twin, was born via emergency C-section. They weighed one pound, four ounces each, and they looked like the babies I had seen on the anti-abortion billboards near the Florida-Georgia line. It was just past the halfway point of my pregnancy—the cusp of viability—and there are many hospitals that would have told me there was nothing they could do. I was not in one of those hospitals, though.
On December 21, 2019, I rolled out the doors of a hospital for women and babies . . . without my babies. I cried as I watched fathers load babies in car seats into the backseat with their mothers. The valet closed the car door, and we pulled out of the loop for the first of 224 times.
On our 7th visit to the Neonatal Intensive Care Unit, a surgeon met with us in the waiting room. “I may open them up and find there’s nothing I can do,” he said. Both girls had suffered bowel perforations—a death sentence for 50 percent of babies with the same diagnosis. The surgeon performed this surgery on three babies that day; only two had come back to the NICU.
On our 10th visit to the NICU, a nurse told us she found two white spots on my daughter’s back. “It’s probably nothing, but we are going to biopsy it, just in case.” It wasn’t nothing. It was a flesh-eating fungus that ate all the way to the muscle before the medication started to work.
On our 11th visit to the NICU, our other daughter tested positive for the same fungus.
On our 175th visit to the NICU, my husband watched one of our daughters die.
He watched doctors, nurses, and respiratory therapists storm the room to work on her. When you’re waiting to find out if your baby is dead, 45 seconds feels like a cave dive, void of light and oxygen; it distorts your perception of time. We did not suffocate that day. The chest compressions that broke her rib, saved her life.
RELATED: In the NICU You Proved You Were Tiny But Mighty
On my 200th visit to the NICU, I walked past the bus stop on my way to the car, and I saw a petite woman with a 35-weeks-pregnant belly standing at the bus stop with a cigarette balanced between her fingers. With all the strength of cooked pasta, I made it to my car and slammed the door. The sound that escaped my lips was feral. I took my vitamins and went to every prenatal appointment. I was young, with no pre-existing conditions. I ate my vegetables and took naps; yet, a woman smoking a cigarette would carry her child to term, and I could not. The car reverberated with my guttural cries that, like my daughters’ prematurity, I could not control.
On our second day home from the NICU, we had a doctor’s appointment. I packed a bag with six diapers, a pack of wipes, two changes of clothes, extra pulse oximeter tape, and extra g-tube pads. I filled up the feeding bag with fortified milk and packed the feeding pump into its carrier. I disconnected each baby from her respective oxygen concentrator and connected her to a portable oxygen tank.
I buckled them into their seats and checked half a dozen times that I had done it right. The neighbors looked on while I loaded the tangled mess of tubes and babies into my car, only to have one baby covered in diarrhea before I could put the car in reverse. I unloaded her, changed her, and returned her to her spot beside her sister.
I took a deep breath, put the car into reverse, and backed into a terra-cotta planter.
My therapist once told me you can’t make an appointment with grief. My grief showed up in the driveway that day.
I grieved the motherhood I had imagined—a motherhood with trips to the park in matching outfits and bows in their hair. I mourned the lifetime of appointments with specialists that lay ahead. My heart ached for the day they would become self-conscious of the scars across their bellies.
That day in the driveway, I felt the brokenheartedness that had been there all along, and then I dug deep for bravery and took them to the doctor.
On our 361st day home from the NICU, I strapped two beautiful toddlers in matching outfits and hair bows into their car seats. All the tubes were long gone and a mouth full of teeth were now doing the job that was once the g-tube’s responsibility. I pulled into the hospital parking lot, loaded them into their stroller, and we made our way into the hospital.
“Happy to see you, though I wish it wasn’t in the hospital,” said the security guard, who had greeted us every weekday of our NICU stay.
“Oh, it’s just routine bloodwork,” I said, implying there was nothing to worry about. I was worried, though. I worried they wouldn’t find a vein because we’d used them all up to keep them alive. I worried we would have to wait hours for the vascular team to bring an ultrasound machine to find the vein. I worried the bloodwork results would reveal malabsorption or something worse.
Two phlebotomists poked one of my daughters six times. They wrapped the extra thick rubber band around her little arm and asked me to hold her down. Her screams were full of a fear I could feel in my bones. I was sweaty and teary-eyed when I told them we had had enough. They didn’t get blood that day. We would have to reschedule—we would have to do it all again. With a brave face, I wheeled the twins back to the car, loaded and buckled them, and drove home.
RELATED: To the NICU Mom Who’s Back at Home
My mom opened the door for us, and I sat on the front porch and cried. I cried because full-term, healthy babies don’t have to get bloodwork, but my kids did. I cried for all the ways prematurity had robbed me and my fellow micro-preemie mothers, and I cried because, against all odds, we get to go to the doctor, we get to attempt blood draws, and we get to put bows in their hair.
Prematurity could have taken everything from us, but it didn’t.
It’s Prematurity Awareness Month, and of course, I want you to give all your money to preventing preventable prematurity. I want you to support hospitals that will intervene at 22-weeks gestation. I want you to share this story with your friends, and I want you to stand with me and every mother who did her best but still ended up sitting in a NICU with her whole heart in a plastic box.
Notice the scars of our trauma—the way we check for cars 318 times before crossing the street with a stroller, and the way we tear up when our babies meet basic milestones like bringing their hands midline or lifting their heads during tummy time. I want you to see us and know us because should prematurity ever leave you or someone you love robbed and brokenhearted, we will be here for you.