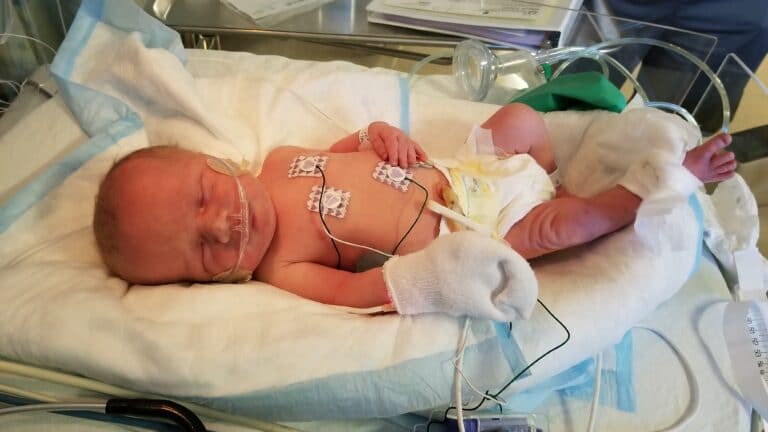
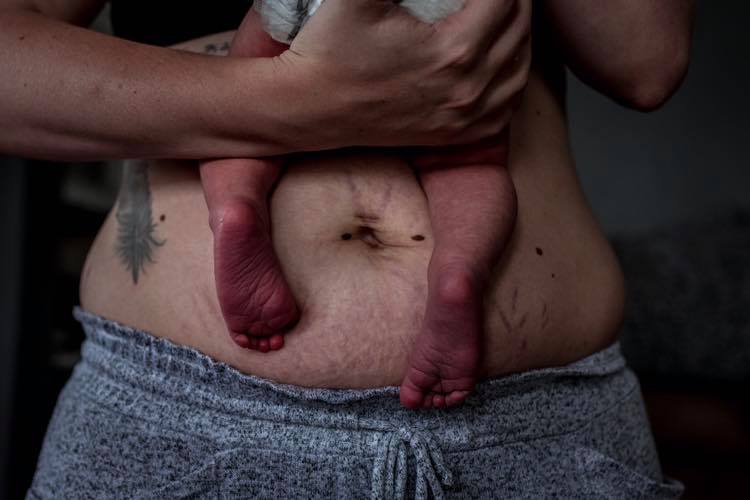
I’ve written before about how it felt to leave my baby for the first time in the NICU.
But somehow, that becomes the norm. Somehow, I developed a routine and just kept going until it felt like that’s all I’ve ever been doing.
Wake up. Pump. Get dressed. Make a smoothie. Pack a lunch. Pack my pump supplies. Drive to the hospital. Pump. Be with my son. Pump. Eat lunch. Be with my son. Pump. Somehow tear myself away and cry driving home. Pump. Eat. Sleep.
Every day for five weeks, that was our lives.
I got there by 8 or 8:30 a.m. every day and got an update from the nurses and sometimes the neonatologist on how my baby was doing. We’d talk about how much weight he’d gained, his breathing status, and other essential vitals. It became the norm to cheer on weight gain of an ounce or two. We celebrated the progress in breathing treatments from CPAP to nasal cannula to room air.
Then for the rest of the day, it was just us.
For three weeks of our five-week NICU stay, he was the only baby being taken care of in the NICU. While this had a lot of pros, including a full nursing staff that only had to focus on one baby, it was not without its cons.
RELATED: Your Heart Never Truly Leaves the NICU
Even with a few nurses around, the NICU was an incredibly lonely place. And when you are in an environment where you are by yourself, you tend to think you are the only one going through this situation. Nobody else could possibly understand what you are going through. My husband was at work all day, and visitors were limited to protect the fragile babies (or in our case, my baby.)
I was allowed to hold my baby skin to skin for a maximum of 60 minutes a day for the first four weeks with the nurse’s permission. We had to coordinate the best time of day to do it so as not to disturb him, and to allow him to get as much rest as possible. Every three hours, the nurses checked him, and I changed his diaper through the isolette. It was usually in the late morning before lunch that I got to hold him, and I’d let the nurse deal with all the wires as she passed him gently to me. I know the act of holding your baby, especially skin to skin, should help with bonding.
But to be honest, it was hard to feel anything but exhaustion, anger, stress, and fear.
No, I didn’t have a baby at home, but I was still up every 2.5 hours pumping at night so I didn’t lose my milk supply.
Yes, I had a whole team of nurses and doctors taking care of my baby, but they made significant errors and mistakes and decisions that I was not comfortable with.
Yes, I was in a hospital setting surrounded by health professionals every day, but nobody ever asked me if I was OK. Not once.
Not even when the neonatologist called me at home at 9 p.m. to report that a nurse made a mistake and pushed 24 hours of lipids in 10 minutes, and that it could essentially clog an artery to his heart or lungs and be fatal. We’d just have to “wait and see.”
Not even when a nurse purposefully pinched my son hard just to see if he’d “open his mouth wider” to attempt to nurse.
Not even when it was me who found the spinal dimple on his back when bathing him, knowing that it was some type of spinal deformity.
No wonder I’d cry every night on my drive home, sometimes needing to pull over because I couldn’t see.
No wonder I developed postpartum depression, anxiety, and PTSD.
It doesn’t matter how supportive your friends and family are, watching your baby go through trauma every day, essentially in an isolated environment is horrific.
Why was I not screened for postpartum mental health disorders?
Why are all NICU moms not automatically screened by a psychiatrist in the hospital during the NICU stay? On a regular basis?
Why are all moms not automatically screened by a psychiatrist on a regular basis?
RELATED: “I Know How Hard She Fought.” Postpartum Depression Claimed Her Life—But Not Her Legacy
My story is not unique. I am one of the 14% of women who suffer from a postpartum mental health disorder. I am one of the 10-15% of moms whose baby requires NICU level care.
I am NOT alone.
My message to you is, and will always be, to educate yourself on ante-natal mental health disorders. Know the signs and symptoms. Make a plan with your spouse, your parents, or your close friends to screen you for it regularly. Ask your OB to screen you. Your child’s pediatrician. Make an appointment with a psychiatrist or psychologist. You don’t deserve to have it be missed.
Even if you had a typical delivery, if your baby was born healthy, if you have no other risk factors–screen yourself. You don’t have to say “well my story isn’t as traumatic as hers, so this couldn’t be postpartum depression/anxiety/PTSD/OCD . . .” Every story is unique. Your feelings are valid.
Disclaimer: This is not medical advice. If you are in a medical emergency, call 911.
Postpartum Support International: Call the helpline at 1-800-944-4773 (#1 En Español or #2 English) The PSI HelpLine does not handle emergencies. People in crisis should call their local emergency number or the National Suicide Prevention Hotline at 1-800-273-TALK (8255).