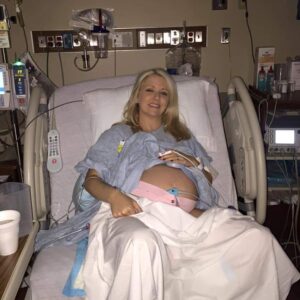
I never expected to be absent during my (possibly only) biological birth. And even if it isn’t my only birth experience, the loss will remain.
Having served families for years as a doula and birth photographer, I was a lover of birth. Each and every time those babies landed on their mama’s chest, oxygen filling lungs and tears spilling out of eyes, I longed for my own birth experience. I supported families in their homes, at birthing centers, in hospitals; I even had the honor of witnessing a cesarean.
After over a year of trying to get pregnant—darn you endometriosis—I finally saw those bright, parallel lines show up on my pregnancy test. I was ecstatic. Within days, my miscarriage began.
We were already pursuing adoption—planned long before our marriage and struggle to conceive—but my burning desire to experience the miracle of pregnancy, labor, and delivery stemmed from serving so many women before me. I dreamed of a home birth, knowing my blood clotting disorders made me high risk.
We grieved that baby-gone-too-soon, continued our adoption pursuit, and prayed for two babies by Christmas 2016.
When we discovered another babe in my womb, we began planning a home birth. Less than four months later, we heard about our son and his need for a family; I was 20 weeks pregnant and unsure his first mom would like that, but we offered ourselves to her anyway. Within hours, we flew across states to meet our firstborn son. I was l bummed to have missed his birth, but knew loss is infused in adoption.
During the course of our high-risk pregnancy, I was open-handed when it came to the possibility that we may need to transfer to a hospital in the case of my blood not clotting or clotting too much. What didn’t even cross my mind, was the reality that I could end up with a Cesarean. It didn’t cross my mind because I was not scared of birth whatsoever; our biological son was considered healthy, and though I was high-risk, I was on lifesaving medication that prevented many disastrous outcomes.
I was so excited to experience and conquer labor and delivery; I knew how to breathe through contractions and the importance of staying present in each moment.
When labor started early on a Tuesday morning, our family’s adrenaline picked up. By the afternoon, our midwife and her team arrived—I had been in active labor with double-peak contractions for over eight hours. The birthing pool was set up in our tiny duplex living room, I was doing the miles circuit with the hope to move baby out of an asynclitic position.
By Wednesday morning, my contractions slowed and we prepared for transition. My contractions never transitioned, they instead remained intensely irregular. After working through 12 incredibly irregular and difficult laboring hours—after 28 hours of active labor already—we made the decision to transfer to a hospital. Nothing we did changed my contractions. Baby’s head was incredibly swollen, making it difficult to find his exact position. We figured after 40 hours of labor, 12 of those hours being irregular, it was time for some pitocin and an epidural. Maybe some rest after all that hard work?
We checked in. The labor and delivery unit was full and out of wheelchairs, so I slowly walked and breathed through contractions, stopping as needed, down the long corridors to the elevator. We settled into our new room as Wednesday passed into Thursday.
I was hopeful for rest through an epidural, but my body never allowed it to work. It metabolized its medicine. They inserted a second epidural, along with more pitocin: my body was refusing to cooperate.
By 6 a.m. Thursday, the doctor told me to prepare mentally for a Cesarean. Why had I not prepared mentally before this moment? The information smacked me in the face as I sat in my bed silently crying, sure this was not my birth story. I was going to push this baby out. I was going to have him placed on my chest with a rush of hormones and emotions, tears flooding the eyes of everyone; I was not going to be high on drugs.
After an ultrasound to confirm Baby’s position as asnclitic, they suggested we try pushing. Maybe he’ll turn and twist and change position. After walking around—hello failed epidural—and squatting and pushing on my hands and knees and vomiting and doing all the hard work a mama can do for over four hours, it was suddenly 5 p.m.
My midwife had remained by my side this entire time. She gently told me to take a break, Baby wasn’t changing position. A few minutes later, she told me she’d never seen a mama fight as hard as I’ve fought, “And that’s saying a lot, Natalie. You know how many births I’ve served.” It was time for my Cesarean; babies aren’t meant to stay in the womb forever and we needed to get him out before he went into distress.
I was so proud of how hard I had worked, how strong I had been, how long I had attempted. Peace washed over me as I accepted that this is what needed to happen and I would still have that magical meeting moment. Sure, the hormones would be a bit drugged and I may be loopy, but the moment would still bring relief and joy and life. I clung to that moment.
I signed papers. They transferred me from bed to cold table. My husband and midwife scrubbed down. The anesthesiologist told me about the medication he was distributing through my epidural catheter. “But what if my body metabolizes it, too?” I asked, nervous about knives cutting into my flesh. “Oh, it won’t. Rarely does that happen. If it does, we will give you a spinal.” He shared some incredibly small percentage of people needing a spinal. My gut told me to prepare myself.
As I expected, my body didn’t accept the typical numbing medication. The anesthesiologist moved on to the spinal, as quickly as he could, Baby was showing signs of distress; he’d been working hard, too. We soon realized the spinal also wasn’t going to work. My body was not accepting any numbing medication, once again not cooperating.
In a flurry, they pushed my midwife and husband out of the room. I heard fast beeping. The shuffle of the room was overwhelming, the bright light, the hands entering spaces of my body I wasn’t prepared for. A gas mask was placed over my face and all went black.
I woke up screaming.
I didn’t recognize anything, had no idea where my husband and newborn were, and a nurse was pushing down on my newly-stitched, eight layers of sliced midsection. “STOP! STOP! WHAT ARE YOU DOING!?” I screamed, tears streaming down my face. I wanted to die.
“Honey, I have to do this to ensure your blood doesn’t clot. The numbing medication didn’t work, and I am so sorry, but I have to do this.” She was kind but I hated her. It felt like a thousand swords were being shoved through my midsection. “How often and for how long?” I begged.
“Every 15 minutes, for maybe three hours.”
I laid there wincing, moaning, sobbing. I saw my husband carrying a bundle toward me, and I wept that I wasn’t ready to meet him, not like this. I didn’t want him to meet me in such a traumatic way. But Baby was hungry. My midwife hooked him up to me for his first feed while I tried to fall back into the haze the drugs had me in; the pain of pushing on my midsection made me desperate to escape.
I later learned our son had to be resuscitated.
The first few days were hazy, gloomy. Postpartum depression settled in right next to this incredibly humbling gratitude that I got to be two babies’ mama. Two within five months.
My healing journey continues. We are coming up on two years since his extraction, and the sadness still permeates my memories. My heart says, likely, there will always be sorrow in the way I met my second born—and that’s OK.
Cesareans are not the easy way out.
Cesareans are difficult to heal from, physically and often emotionally. Months of physical therapy and medication later, my body is dealing a bit better. I have damaged nerves and shooting pains. My body is triggered when I hear others talk about their birth experiences.
I’ve learned that no matter our birth experience, there is room for both sorrow and joy, sadness and gratitude. No matter how much we prepare for and know about and love birth, we still cannot control it. And no matter how prepared you may be for one, they’ll still scar you for a lifetime.
So as you continue on in your journey and what you know about Cesareans, know that they aren’t easy. They aren’t fun. But they don’t make you any less of a mother.
I am not ashamed of having a Cesarean. I don’t believe birthing a child in ANY way, or at all, makes me more or less of a mother.
I am grateful Ira is in my arms and I get to celebrate his life. Incredibly grateful, every single day.
The most broken pieces of our heart show our great capacity to love. So let me sit in the sad parts when I need to; I know Jesus sits with me right there in the pain, showering me with grace.